Many people diagnosed with a substance use disorder also have a co-occurring mental health disorder, such as anxiety, depression, or post-traumatic stress disorder (PTSD). Substance addiction and mental health conditions interact in a complex way, so specialized treatment is pivotal if you are seeking help for a dual diagnosis.
In this article:
- What is Dual Diagnosis?
- How are Addiction and Mental Health Related?
- Dual Diagnosis Self-Assessment Quiz
- What is Dual Diagnosis Treatment?
What is Dual Diagnosis?
A dual diagnosis commonly refers to a substance use disorder (SUD) that is also diagnosed with a mental health condition. Also termed co-occurring disorders, a mental health and substance use disorder diagnosed together often require inpatient rehab treatment for the best chances of recovery success.
What Are Some Common Co-Occurring Disorders?
Having a dual diagnosis is common if you have a substance use disorder. In fact, a 2018 Substance Abuse and Mental Health Services Administration (SAMHSA) study on drug use and health reported that approximately 9.2 million adults have co-occurring mental health and substance use disorders.²
Co-occurring disorders may include any combination of mental health diagnoses in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR).³ There are no exclusive co-occurring disorders with a SUD. A dual diagnosis may include any SUD plus a mental health diagnosis in the DSM-5-TR. However, some mental health conditions are more common in dual diagnosis with addiction, including:⁴ ⁵
- Trauma or other stressor-related disorders (including post-traumatic stress disorder, PTSD)
- Anxiety disorders (such as generalized anxiety disorder and panic disorder)
- Depressive disorders (such as major depressive disorder)
- Mood disorders, such as bipolar I and II disorders
- Attention deficit hyperactivity disorder (ADHD)
- Schizophrenia or other psychotic disorders
- Borderline personality disorder (BPD)
- Antisocial personality disorder
According to NIDA’s 2023 Survey on Drug Use and Health, here are the 10 most common mental health conditions that co-occur with addiction and substance use:
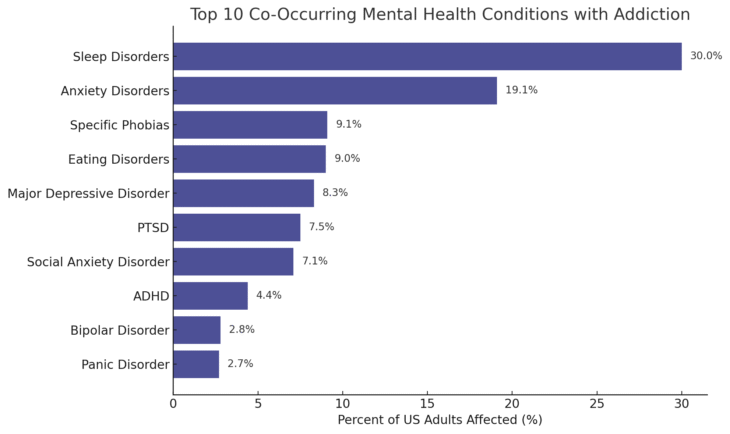
Just because you have one of these mental health conditions does not mean you will necessarily develop a substance use disorder. These co-occurring disorders are correlated, not causal.
Several national studies have found that about half of people with SUDs or mental health disorders have the other as a co-occurring disorder.⁵ There are shared risk factors for mental health and an alcohol or substance use disorder.
Risk factors for addiction include:⁵
- Substance use or mental health disorders in childhood or adolescence increase the risk of having one or the other.
- People with a mental health condition or substance use disorder have a higher risk for non-medical prescription opioid use.
- Untreated ADHD in childhood increases the risk of a SUD later in life.
- Genetic and epigenetic susceptibilities overlap between the co-occurring disorders.
- Similar brain areas are impacted by mental health conditions and substance use disorders (such as reward centers, impulse control, and decision-making).
- Several neurotransmitters are involved in both mental health conditions and substance use, including serotonin, dopamine, GABA, glutamate, and norepinephrine.
Additionally, certain environmental factors or stressors increase the risk of a dual diagnosis. These include trauma, chronic stress, and adverse childhood events (ACEs). Often these events are interrelated with self-medicating or drug or alcohol use, which can lead to changes in the brain.
For instance, someone with PTSD may begin using alcohol to get rid of intrusive memories of their trauma. Even more, using cocaine may increase the symptoms of bipolar disorder.
If you have a genetic predisposition to a mental health condition, then using certain substances may produce changes in the brain that trigger the predisposition to developing a mental health condition. Using alcohol or drugs while having a mental health condition has been shown to enhance the rewarding effects of the drug, decrease awareness of the negative effects, and alleviate some of the mental health symptoms.⁵
Dual Diagnosis Self-Assessment
If you’re wondering whether or not you might have a clinical dual diagnosis, there are a couple of questions you can ask yourself to determine whether or not you should consider talking to a health care provider. Keep in mind this self-assessment is not medical advice and should not be considered as any kind of diagnosis – only your own medical professional can give you that.

To complete the dual diagnosis self-assessment:
- For each question above, rate how often the question is true in the past 6 months
- 0 points if never true and does not apply, up to a max of 3 points if the question is always or almost always true
- Add up the points from each answer to get a total out of 18
If you scored 10 or more points, you may want to talk to your health care provider about your substance use and mental health patterns.
If you’d like to learn more about dual diagnosis treatment for addiction but don’t know where to start, you’re not alone.
Call
800-914-7089
(Sponsored)
to talk to someone about your treatment options.
What is Dual Diagnosis Treatment?
Treating dual diagnoses can be difficult, as it can be hard to separate the symptoms of the co-occurring disorders or figure out which came first. Dual diagnosis treatment means treating both addiction and mental illness together. It is crucial for someone with co-occurring conditions to receive dual diagnosis care to have the best possible treatment outcome.
Research has shown that treating co-occurring disorders simultaneously leads to better success than treating them separately.⁵ This type of treatment typically consists of a team working together to treat an individual through individual therapy, group therapy, and medication management. It is always recommended to seek inpatient treatment at a facility that specializes in dual diagnosis treatment.
Types of Therapies Used in Addiction Treatment
There are many facets to effective treatment programs, but evidence-based behavioral therapy has proven especially effective in treating co-occurring disorders. Medication management alongside therapy is typically the recommended standard of treatment for co-occurring disorders. Also, specific therapies have shown better outcomes for certain dual diagnosis treatments.
Some of the most common types of therapy used in addiction treatment include: ⁵
- Cognitive Behavioral Therapy (CBT): CBT is effective for children and adolescents with co-occurring substance use and anxiety or depression. A therapist trained in CBT can help you address and reframe your thoughts and behaviors with short-term treatment goals.
- Dialectical Behavior Therapy (DBT): DBT is designed to help people with destructive behaviors and negative thinking patterns. It is one of the most effective treatments for borderline personality disorder (BPD) and has also been proven beneficial for many other disorders.
- Contingency Management (CM) or Motivational Interviewing (MI): CM or MI use incentivized based treatments to help reduce unwanted behaviors. These incentives are integrated into treatment programs and can help motivate change.
- Exposure Therapy: Exposure therapy treats certain anxiety disorders, such as PTSD or phobias. The goal is to expose yourself to the stimulus that makes you anxious, and in the long run, it’ll reduce the anxiety you feel.
- Integrated Group Therapy (IGT): IGT treatment is CBT-based therapy specifically for people with a dual diagnosis of bipolar disorder and substance use disorder. It helps teach recovery and relapse prevention skills that help both diagnoses.
Additional treatments in dual diagnosis programs may include:5
- Assertive Community Treatment (ACT): ACT uses individualized case management and behavioral treatments for serious mental illnesses like schizophrenia and substance use disorders.
- Therapeutic Communities (TC): TCs are long-term residential treatments that have been shown to be helpful with certain populations, such as adolescents, individuals with a criminal history, or individuals dealing with homelessness. Community-based and “resocialization” approaches are often used as part of treatment.
- Seeking Safety (SS): SS is a treatment aimed at treating dual diagnosis trauma and substance use. Present-oriented and behavioral skills are taught in the treatment.
- Mobile Medical Application: This mobile app provides CBT treatment in conjunction with other treatments to help people with substance use disorders.

Types of Therapy Used in Addiction Treatment
Learn about evidence based therapy approaches like CBT, motivational interviewing, and pharmacotherapy address the root causes of substance use. Explore how personalized treatment can help you or a loved one regain control.
Read more.
Treatment at Rehab
Having a dual diagnosis can be complicated since you likely have symptoms that overlap with other disorders, which may also affect or heighten one another. There are several program types for dual diagnosis treatment options: coordinated, co-located, and fully integrated.
A fully integrated dual diagnosis treatment program is the preferred way for someone with co-occurring disorders to achieve recovery.⁶ This can be best achieved in an inpatient dual diagnosis rehab setting. This setting allows for a fulsome, team approach, where treatment interventions are actively combined to address both disorders together.⁷
These facilities create treatment plans tailored to the specific mental health disorder you are diagnosed with and the substance you are misusing to help you achieve recovery and manage symptoms effectively.
Finding Dual Diagnosis Specialists
Finding a dual diagnosis treatment center that provides evidence-based treatment and fully integrated care is important to help you succeed in your recovery. Our rehab center database can help you find treatment centers across the U.S. Additionally, you can contact your primary care doctor, a mental health professional, or your insurance provider for referrals or suggestions.
Call
800-914-7089
(Sponsored)
today to learn more about dual diagnosis rehab facilities near you.
Addiction Treatment Resources

What to Expect From Inpatient Drug Rehab
Inpatient rehab provides 24/7 support in a structured environment, helping individuals focus fully on recovery through medical care, therapy, and daily routines tailored to addiction treatment.
Read more.
Medical Detox for Drug & Alcohol Addiction
Drug detox programs safely manage withdrawal symptoms under medical supervision, serving as a critical first step in the recovery process before entering rehab or long-term treatment.
Read more.

When Does Outpatient Drug Rehab Make Sense?
Outpatient rehab offers flexible, part-time treatment for addiction, allowing individuals to maintain work or family commitments while attending therapy sessions and support groups regularly.
Read more.

What is Sober Living and How Does it Work?
Sober living programs offer a supportive, drug free environment for individuals transitioning from rehab, helping to build accountability and independence in early recovery.
Read more.
Follow Us
Resources
- Substance Abuse and Mental Health Services Administration. (2022, April). Mental Health and Substance Use Disorders.
- Substance Abuse and Mental Health Services Administration. (2010). Key Substance Use and Mental Health Indicators in the United States: Results from the 2018 National Survey on Drug Use and Health.
- American Psychiatric Association. (2022, March). Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision. American Psychiatric Association Publishing.
- Substance Abuse and Mental Health Services Administration. (2022). Co-Occurring Disorders and Other Health Conditions.
- National Institute on Drug Abuse. (2021, April). Part 1: The Connection Between Substance Use Disorders and Mental Illness.
- National Institute on Drug Abuse. (2024, September). Co-Occurring Disorders and Health Conditions.
- Substance Abuse and Mental Health Services Administration. (2021). The case for screening and treating co-occurring disorders.
- Substance Abuse and Mental Health Services Administration. (2022). TIP 42: Substance Use Treatment for Persons With Co-Occurring Disorders.


